The December 2025 newsletter features updates on the PHAGE and DOTS (Dalbavancin as an an Option for Treatment of Staphylococcus aureus bacteremia) studies as well as a clinical trial site spotlight on the University of North Carolina. The newsletter also includes a mentee spotlight, study milestones, recent publications, and more ARLG network news.
Author: AM
ARLG Steering Committee Members Receive Recognition for Significant Contributions to AMR
Congratulations to the ARLG Steering Committee members who received recognition as one of Clarivate’s Highly Cited Researchers in 2025! Clarivate uses a meticulous process to identify researchers who have significantly influenced their fields during the past year. Learn more about the important work these leaders in antimicrobial resistance are doing to improve patient care by advancing the prevention, diagnosis, and treatment of infections caused by antibiotic-resistant bacteria:
PHAGE Trial Reached Database Lock
We are pleased to announce that the PHAGE study has successfully reached database lock. This Phase 1b/2 clinical trial investigated the safety profile and microbiological activity of bacteriophage therapy in individuals with cystic fibrosis (CF) who are chronically colonized with Pseudomonas aeruginosa.
Led by Pranita Tamma, MD, MHS, University of Pennsylvania, and Robert Schooley, MD, University of California, San Diego, the trial enrolled 72 participants across 17 sites. Participants were randomized to receive either a single intravenous dose of a four-component bacteriophage cocktail or a placebo.
The data generated from the PHAGE study will deepen our understanding of optimal dosing strategies, safety considerations, and the expected microbiological responses associated with bacteriophage therapy. Importantly, these findings will guide the design of future clinical trials that aim to advance bacteriophage-based treatments for antimicrobial-resistant infections, extending beyond P. aeruginosa-related lung disease.
For additional details, consult the study record—and stay tuned for forthcoming results.
ARLG Fellow Natalie Mackow, MD, MSCR, Receives SHEA Trainee Award at IDWeek

Congratulations to ARLG Fellow Natalie Mackow, MD, MSCR! Dr. Mackow received the SHEA Trainee award at IDWeek 2025 for her abstract, “Using a novel Anaerobic Activity Index to assess risk for poor outcomes in burn patients in a burn intensive care unit.”
Dr. Mackow’s research aims to inform antibacterial therapy practices in patients with severe burns to reduce the prevalence of antibacterial resistance, which may be applicable to prevention approaches in other critically ill patient populations.
“Systemic antibiotic therapy is an important, potentially modifiable, risk factor for antibacterial resistance in this vulnerable patient population,” says Dr. Mackow. “Additionally, a novel tool to improve our definition of the anti-anaerobic activity of antibacterials has the potential to be utilized broadly in clinical studies and clinical practice, once validated.”
Learn more about Dr. Mackow’s research and how an ARLG Fellowship supported her work to improve outcomes for patients with severe burns in her ARLG Mentee Spotlight.
DOTS Study Results Discussed in NEJM Journal Watch
In a recent article, “DOTS: Optimism Around a ‘Negative’ Dalbavancin Trial,” Dr. Paul Sax summarizes the results of the DOTS study and why the findings are important.
Researchers for the DOTS study wanted to learn if two doses of dalbavancin, a long-lasting antibiotic often used to treat severe, bacterial skin infections, could work better than the standard peripherally inserted central catheter (or PICC line) antibiotic treatment for patients hospitalized for complicated Staphylococcus aureus bloodstream infections. The study results showed that although dalbavancin was not better at treating bloodstream infections, it worked as well as the standard therapy with fewer patients having to stop or change treatment due to side effects.
“So yes, DOTS was ‘negative’ on its primary outcome,” said Dr. Sax. “But it also showed that dalbavancin performs about as well as what we do now, with far less infrastructure: no PICC, no daily infusions, no vancomycin levels, fewer moving parts.”
Learn more about these important findings to improve patient outcomes for antibiotic-resistant infections in the ARLG news and the DOTS Summary of Results.
ARLG at IDWeek 2025
IDWeek 2025 is here! Whether you’re attending in person in Atlanta, GA or online, you can hear some of ARLG’s top leaders and experts discuss the latest AMR topics.
You won’t want to miss this year’s SHEA Lectureship, which was awarded to ARLG’s Mentoring Committee Chair, Anthony Harris, MD, MPH. This award recognizes his important contributions to the fields of health care epidemiology, infection prevention, and antimicrobial stewardship through his leadership and mentorship. Dr. Harris will give his lecture, “Where is the true north of infection control?” on Tuesday, October 21 at 4:45 p.m. ET.
Check out the ARLG member sessions and presentations in the tables below, or view the full schedule and on-demand content at IDWeek.org.
Sessions
| Day | Time (ET) | Session Title | Presentation Title | Moderators | Speakers |
|---|---|---|---|---|---|
| 10/19/2025 | 10:45 - 11:30 am | PW07 – Expanding Your Influence to Improve Antibiotic Use in Outpatient Settings | Advancing Outpatient Stewardship in Health Systems | Ritu Banerjee | |
| 10/19/2025 | 10:50 am - 12:15 pm | PW04 – Fellows’ Day Workshop | Careers in Research | Cesar Arias | |
| 10/19/2025 | 2:40 – 3:15 pm | 2 – Beyond the 101: Pondering Perplexing Prescribing Issues | Can We Use Ceftriaxone Susceptibility to Interpret Susceptibility to Third-Generation Cephalosporins? | Pranita Tamma | |
| 10/19/2025 | 3:45 – 5:30 pm | 8 – Opening Plenary: Reflection and Renewal: Advancing Public Health in Challenging Times | Yohei Doi | ||
| 10/20/2025 | 8:00 – 9:00 am | 15 – New Antimicrobials in the Pipeline | David van Duin | ||
| 10/20/2025 | 8:00 – 8:30 am | 17 – These Blind Mice: When Bench Doesn’t Meet Bedside | Optimizing Dosing Strategies: Insights From Systems Pharmacology and Experimental Models | Gauri Rao | |
| 10/20/2025 | 8:00 – 9:00 am | 18 – Top 10 Papers in Antimicrobial Resistance | Yohei Doi | ||
| 10/20/2025 | 10:55 - 11:20 am | 24 – Applying Next-Generation Sequencing to Clinical Treatment and Prevention | Cases in Genotype-Phenotype in the Microbiology Laboratory: What Clinician Need to Know | Amy Mathers | |
| 10/20/2025 | 10:30 - 11:45 am | 25 – Blood and Guts: Microbiome Discoveries | David van Duin | ||
| 10/20/2025 | 10:30 - 11:45 am | 30 – Lessons Learned in Biopreparedness and Biocontainment: Lassa Fever in the Midwest | Yohei Doi | ||
| 10/20/2025 | 2:21 – 2:39 pm | 64 – Out With the Old, in With the New: Time to Update the Management of Staphylococcus aureus infections | Should Ceftobiprole Replace Ceftaroline in the Management of Persistent Staphylococcal Bacteremia? | Nicholas Turner | |
| 10/20/2025 | 1:45 – 3:00 pm | 72 – Late Breaking Trial Results for Viral and Bacterial Infections | Yohei Doi | ||
| 10/20/2025 | 3:15 – 4:30 pm | 84 – Diagnostic Clinical Cases: What Do I Do With This Test Result? | Ritu Banerjee | ||
| 10/20/2025 | 3:15-4:30 pm | 87 – Extra, Extra New Info on Treating and Preventing RSV and Influenza | Angelique Boutzoukas | ||
| 10/20/2025 | 3:15-4:30 pm | 88 – New Anti-Infective Agents | Pranita Tamma | ||
| 10/20/2025 | 3:15-4:30 pm | 84 – Commonalities and Differences in Antimicrobial Treatment of Resistant Pathogens | Yohei Doi | ||
| 10/21/2025 | 8:00 – 9:00 am | 99 – Diagnostic Trials: Past and Future | Robin Patel, Ritu Banerjee | ||
| 10/21/2025 | 8:00 – 8:30 am | 99 – Diagnostic Trials: Past and Future | Evaluation of Infectious Disease Diagnostics: Innovative Study Designs to Assess Test Performance | Michael Satlin | |
| 10/21/2025 | 8:30 – 9:00 am | 99 – Diagnostic Trials: Past and Future | Evaluation of Infectious Disease Diagnostics: Study Designs to Assess Impact on Clinical Outcomes | Sarah Doernberg | |
| 10/21/2025 | 8:00 – 9:00 am | 104 – Pediatric Antimicrobial Resistance: Key Updates for the Busy Clinician | Latania Logan, Pranita Tamma | ||
| 10/21/2025 | 8:30 – 9:00 am | 104 – Pediatric Antimicrobial Resistance: Key Updates for the Busy Clinician | Updates in Gram-Negative Bacteria | Angelique Boutzoukas | |
| 10/21/2025 | 9:15 -10:00 am | 107 – Maxwell Finland Lecture | Yohei Doi | ||
| 10/21/2025 | 9:35 -10:00 am | 107 – Maxwell Finland Lecture | Antimicrobial Resistance at the Bedside: Translating Science into Patient Outcomes | Cesar Arias | |
| 10/21/2025 | 1:45 – 3:00 pm | 157 – Cavities, Appys, and CLABSis, Oh My! Perspectives From Our Surgery and Radiology Colleagues | Latania Logan | ||
| 10/21/2025 | 1:45 – 3:00 pm | 162 – Fresh New Results On Old and New Vaccines | Ahmed Babiker | ||
| 10/21/2025 | 1:45 – 3:00 pm | 163 – Lowering Barriers to Diagnostics Access to Reduce Health Inequalities and Improve Outcomes | Ritu Banerjee | ||
| 10/21/2025 | 3:15 – 4:30 pm | 171 – New Antibiotics, Untapped Potential: Exploring the Underuse of Recently Approved Agents | Thomas Lodise | ||
| 10/21/2025 | 4:05 – 4:30 pm | 172 – Bug to Drug: Translating Mechanisms of Antimicrobial Resistance to Treatment of Challenging Infections | Translational Antimicrobial Resistance Research in Low-Resource Settings | Jose Munita | |
| 10/21/2025 | 3:15 – 4:30 pm | 173 – Challenging Cases in Immunocompromised Host | Michael Satlin (panelist) | ||
| 10/21/2025 | 5:25 – 5:55 pm | 183 – SHEA Lectureship | Where is the True North of Infection Control? | Anthony Harris | |
| 10/21/2025 | 4:45 – 6:00 pm | 184 – Stanley A. Plotkin Lecture in Vaccinology | Latania Logan | ||
| 10/22/2025 | 8:00 –8:20 am | 191 – One Size Fits One: Toward Individualized Management of Infectious Diseases | Molecular Diagnostics to Refine Duration of Therapy for Blood Stream Infection: S. aureus | Vance Fowler | |
| 10/22/2025 | 10:30 -10:55 am | 197 – Clinical Trials That Will Change Your Practice | Trials in Bacteriology That May Change Your Practice | Amy Mathers | |
| 10/22/2025 | 1:45-3:00 pm | 241 – Advances in Managing Antimicrobial Toxicities | Amit Pai | ||
| 10/22/2025 | 3:15 – 4:30 pm | 257 – Cracking the Code of Resistance: A Deep Dive Into Metallo-Beta-Lactamase From Bench to Bedside | Yohei Doi, Amy Mathers | ||
| 10/22/2025 | 3:15 – 3:40 pm | 257 – Cracking the Code of Resistance: A Deep Dive Into Metallo-Beta-Lactamase From Bench to Bedside | Unmasking Resistance: Epidemiology and Diversity of MBLs | Maria Mojica | |
| 10/22/2025 | 3:15 – 4:30 pm | 259 – Driving Better Decisions: Incentivizing Diagnostic Stewardship | Ritu Banerjee | ||
| 10/22/2025 | 3:15 – 4:30 pm | 266 – Why Do We Do This? Exploring the Data Behind Long-Established Practices in ID | Double Coverage; Do We Need It? | Kerry LaPlante |
Posters & Oral Presentations
| Day | Time (ET) | Title | Presenting Author | Authors |
|---|---|---|---|---|
| 10/20/2025 | 11:18 – 11:30 am | 78 – Oral Presentation: Aerobactin Gene iuc as a Virulence Marker Associated with Increased Mortality in Carbapenem-Resistant Klebsiella pneumoniae infections: A Multicenter Observational Cohort Study from China | Jianping Jiang | Jiang JJ, Li Y, Komarow L, Boutzoukas A, Yu Y, Xiao Y, Gao H, Liu Z, Fowler Jr VG, Kreiswirth BN, Chen L, Wang M, van Duin D, for the Antibacterial Resistance Leadership Group |
| 10/20/2025 | 12:15-1:30 pm | P-476 – Poster Presentation: Risk Factors for Mortality in Children and Young Adults with Carbapenem-Resistant Gram-Negative Infections | Angelique Boutzoukas | Boutzoukas AE, Tian J, Komarow L, Ge L, Wang M, Arias C, Guttierrez JMO, Alenazi T, Liu Z, Paterson D, Satlin M, Doi Y, Fowler V, van Duin D |
| 10/21/2025 | 12:15 – 1:30 pm | P-1292 – Poster Presentation: Clinical and Genomic Features of Colistin Resistance Among Carbapenem-resistant Acinetobacter baumannii Isolated From Global Clinical Samples | Madison Stellfox | Stellfox ME, Komarow L, Patel R, van Duin D, Van Tyne D, Doi Y |
| 10/21/2025 | 12:15 – 1:30 pm | P-1296 – Poster Presentation: Impact of Metallo-Beta Lactamases on Outcomes in Patients with Carbapenem-Resistant Gram-Negative Infections | Angelique Boutzoukas | Boutzoukas AE, Shao W, Jiang J, Kanj S, Wang M, Salcedo Mendoza S, Marimuthu K, Liu Z, Komarow L, Fowler V, Kreiswirth B, Arias C, Doi Y, Paterson D, Satlin M, Bonomo R, van Duin D |
| 10/21/2025 | 12:15 – 1:30 pm | P-1302 – Poster Presentation: Klebsiella pneumoniae Phage Susceptibility Testing (PST): Comparison Between a Spot Plaque Assay and an Optical Density-Based Liquid Assay | Luz Cuello | Cuello L, Patel R |
| 10/22/2025 | 10:45 – 11:00 am | 556 – Oral Presentation: Using a novel Anaerobic Activity Index to assess risk for poor outcomes in burn patients in a burn intensive care unit | Natalie Mackow | Mackow NA, Komarow L, Napravnik S, Bartelt L, DiBiase LM, Williams B, Williams FN, Weber DJ, van Duin D |
September 2025
The September 2025 newsletter highlights the new ARLG supplement published in the journal of Clinical Infectious Diseases and celebrates the important work of recent retirees who dedicated years of service to the ARLG. This edition of the newsletter also includes a new clinical site spotlight, study milestones, recent publications, and more.
DOTS Study Results Published
 The results of an ARLG study, Dalbavancin as an Option for Treatment of S. aureus Bacteremia (DOTS), were recently published in JAMA.
The results of an ARLG study, Dalbavancin as an Option for Treatment of S. aureus Bacteremia (DOTS), were recently published in JAMA.
In this study, researchers compared the safety and efficacy of dalbavancin to the standard of care in treating patients with complicated Staphylococcus aureus bloodstream infections. Antibiotics for serious S. aureus infections are typically delivered over 4-6 weeks through a central catheter, or PICC line, that requires specialized care and may lead to other complications like additional infections. Results indicate that dalbavancin, delivered in two doses one week apart, can be as effective as the standard of care while avoiding the potential risks associated with a PICC line. These findings are significant because better, safer treatments are needed for S. aureus bloodstream infections, which are common in hospitals and can be deadly.
To learn more about these important findings to improve patient outcomes for antibiotic-resistant infections, read the DOTS summary of results, listen to the JAMA Author Interviews podcast, and check out the Duke Health press release.
ARLG Retiree Spotlight – Beth Evans, Lead Clinical Research Associate

Our best wishes go out to Beth Evans, CCRA, on her retirement after 29 years at Duke Clinical Research Institute (DCRI). Since 2016, she has worked with ARLG as a lead CRA on many studies including HABP/VABP, MDRO, SNAP, CRACKLE-2, POP, SHREC, and PHAGE.
“My passion was to work closely with site personnel, training them and guiding them through the day-to-day study activities,” Beth states. “I loved the details of each study and helping sites understand and follow the protocol. I was often called ‘Eagle Eyes’ for finding details others may have missed.”
In 2021, Beth channeled her passion and expertise into working on the PHAGE study with Drs. Robert “Chip” Schooley and Pranita Tamma to evaluate bacteriophages as a promising alternative to antibiotics. Her experience on the MDRO study as a site manager for the U.S. and Asia-Pacific regions was equally exciting as she traveled to provide study team training at multiple sites across China and Australia. “It was inspiring to see sites across the globe unite on one mission – the fight against antimicrobial resistance,” she states. “Given the growing threat of antibiotic-resistant bacteria, contributing to research that combats this global health issue is very important to me. ARLG is a world leader in the prevention and treatment of infections that could one day directly benefit me or someone close to me.”
Now that Beth has retired, she has no intention of sitting still. She will direct her passion and energy into hiking, paddleboarding, and playing tennis. During the next two years, she hopes to hike the tallest point in every U.S. state. When she isn’t outdoors, Beth plans to spend more time playing piano and may also take banjo lessons.
New ARLG Supplement Published in Clinical Infectious Diseases
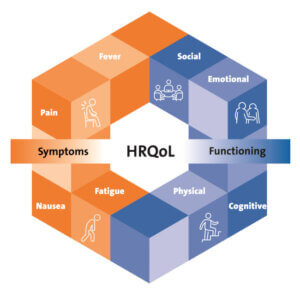 The ARLG published a new supplement in the journal of Clinical Infectious Diseases titled “In Pursuit of Patient-Centered Antibacterial Trials: Listening to, Learning From, and Leveraging the Patient Perspective.” The supplement includes eight articles authored by ARLG members that describe several challenges and opportunities for measuring health-related quality of life (HRQoL) in patient care and in clinical studies of infectious diseases.
The ARLG published a new supplement in the journal of Clinical Infectious Diseases titled “In Pursuit of Patient-Centered Antibacterial Trials: Listening to, Learning From, and Leveraging the Patient Perspective.” The supplement includes eight articles authored by ARLG members that describe several challenges and opportunities for measuring health-related quality of life (HRQoL) in patient care and in clinical studies of infectious diseases.
